Vote safely in person in November. Here are 5 tips to ensure elders vote safely during the 2020 election year.
Dealing with information overload and consistent bad news during the COVID-19 pandemic is crucial to our sruvival. Here's how to navigate it.
The flu season is upon us. Here's how caregivers and the elderly can prepare for the flu season during COVID-19.
Have outside caregivers coming into your home during the COVID-19 pandemic? Here are 5 safety guidelines you should continue to consider.
Do masks prevent COVID-19? Are they effective? What research is there is show how masks prevent COVID-19? Find out in this post.
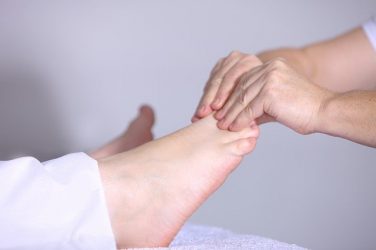
Improving circulation in older adults. Circulation problems are common amongst older adults. Here's how to improve circulation.
Living with cirrhosis: risk factors, life expectancy and tips for caregivers.
Cirrhosis is a serious chronic progressive disease that affects the liver.
The on-going disease destroys the liver cells called hepatocytes.
As the disease progresses, the liver becomes scarred. And this scarring ultimately leads to liver dysfunction.
Although cirrhosis can be managed and slowed down, it is a serious illness that can lead to death.
Living with cirrhosis: what causes cirrhosis?
Most people associate cirrhosis with alcoholism.
And while this is a major risk factor for the disease, it’s not the only reason a person might have cirrhosis.
Other causes of cirrhosis include:
- As a complication of a liver infection (hepatitis)
- Exposure to hepatoxins (or chemicals that are toxic to the liver other than alcohol)
- Severe, right-sided heart failure which results in an enlarged and fluid-filled liver
Thus if you have a loved one who has heart disease or has had hepatitis in the past, these could serve as risk factors for cirrhosis too.
How long can you live with cirrhosis of the liver?
Surviving cirrhosis depends on multiple factors including age, the overall health of the person and the cause of cirrhosis.
Thus how long a person can live with cirrhosis will differ from one person to the next.
There are four stages of cirrhosis.
The four stages of cirrhosis
- During stage 1, patients lack energy and constantly feel tired. The liver is inflamed at this point and the individual may have a swollen abdomen. Cirrhosis can be reversed at this stage if a doctor detects it early and the patient makes the right lifestyle changes.
- During stage 2 of cirrhosis, the pressure in the veins surrounding the liver begin to rise. This happens because of an obstruction in blood flow to the liver. This is called portal hypertension. With reduced blood flow and increasing scar tissue, cirrhosis could be slowed at this stage but it may not work.
- Ascites – or fluid accumulation in the belly area – develops during stage 3 of cirrhosis. At this point, the veins are congested and so a lot of fluid gets trapped in the abdomen. More scar tissue develops in the liver. Other symptoms like itchiness, lack of sleep and weight loss happen at this stage. Jaundice also happens at this stage. Jaundice is a yellowing of the skin and tissues that happens because the liver can no longer break down a substance called bilirubin. At stage 3, cirrhosis is irreversible. And at this point, the individual becomes a candidate for a liver transplant.
- The symptoms associated with stage 3 cirrhosis are similar to stage 4. During the final stages of cirrhosis of the liver, confusion, personality changes and hand/muscle tremors become common.
What can you do as a caregiver?
At stages 1 and 2 of cirrhosis, we can still do a lot to slow down the disease.
You can help your loved one make lifestyle changes like:
- Quitting alcohol
- Exercising regularly
- Eating a balanced diet of meals
- Restricting sodium and fluid intake (especially when ascites starts)
- Following medication regimen that is prescribed by a qualified medical provider
- Quitting opioid and narcotic intake
- And even in following medication regimen, make sure you are reading labels to ensure medication will not harm your loved one’s liver.
During stages 3 and 4, cirrhosis is not reversible.
At this point, you can mainly provide supportive care to your loved one as they wait to get a liver transplant.
- For a loved one who is confused, provide a safe environment so they don’t hurt themselves.
- Elevate the head of the bed while they sleep. This reduces shortness of breath.
- Monitoring your loved one’s level of consciousness.
During these stages, it might be time to consider working with professional caregivers so that your loved living with cirrhosis can get the proper care they need.
What is a durable power of attorney and why do you need one?
We’re living through a pandemic.
It is more important than ever for seniors to think about what kinds of medical decisions you want to be made for you in case you cannot make them yourself.
A medical durable power of attorney is document that gives someone else the power to make decisions on your behalf. Of course, this would be in a scenario where you cannot make those decisions yourself.
Although COVID-19 can affect people of all ages and different demographics have recovered from the illness, it is important for older adults to clearly state in writing, who can make decisions for them in case they’re unable to do so.
Even in the absence of COVID-19, accidents, illness and age-related dementia call for older adults to prepare a durable power of attorney.
Selecting a durable power of attorney for healthcare
Nobody can dictate who you choose as your durable power of attorney.
However, we recommend that you choose someone you trust and who is reliable.
It is best if you can work with a lawyer to draft the legal document when you’re appointing the power of attorney.
Can I name more than one person as a power of attorney?
If you live in the United States, you can name more than one person as your durable power of attorney.
However, it is important to specify exactly what each of their roles in decision-making will be.
And whether or not one decision supersedes another should they have conflicting ideas on a medical decision.
We highly recommend that you have a conversation with your lawyer so you can understand the pros and cons of choosing one or multiple powers of attorney.
What happens after I name my medical power of attorney (POA)?
You will work with your lawyer to draft the legal document.
Once it is finished and all the needed signatures are on your document, you can save the document in different places.
- Your lawyers will have a copy.
- You can save a copy in your home in a place where your spouse or named power of attorney knows.
- If you have a personal doctor, you could also ask them to keep one with your medical records.
Having a durable power of attorney long before you need it, can prevent family misunderstandings.
And it will prevent a court of law (instead of your loved ones) from making crucial medical decisions for you.
Also note that, a POA may be called a “healthcare proxy”, “agent” or “healthcare surrogate” depending on where you live.
Read this post where we talk more extensively about estate planning for older adults.
Your elderly loved one is bleeding from the nose and you are worried.
What could be the issue? Why are they experiencing nosebleeds so much?
Nosebleeds in the elderly can happen for the following reasons.
- Dry weather that dries up the nostrils
- Sinus infection
- Aspirin use (if your loved one takes aspirin as part of their medication regimen)
- Blood thinners
- A foreign body in the nose
- Allergies
- Even nasal sprays that treat allergies can also cause nosebleeds
Most of these are not a cause for alarm. And usually, you can resolve a nosebleed by getting rid of the precipitating event.
For most older adults, an occasional nosebleed may be nothing to worry about.
But regular nosebleeds for an older loved one could point to more serious issues like a severely injured nose (due to a fall or another type of accident), coagulation disorders, heart problems, arterial hypertension and some types of cancers.
To stop a nosebleed:
- Get your loved one to sit down and lean forward.
- Pinch the soft part of their nose (or direct them) just above the nostrils and hold it for 10 to 15 minutes.
- You can also place an ice pack wrapped in a towel (or frozen vegetables) over the bridge of their nose.
If a nosebleed lasts for longer than 20 minutes, you should seek immediate medical attention.
Nosebleeds in the elderly – what you can do as a caregiver
Like I mentioned before, you can treat occasional nosebleeds by treating what caused it. Here are steps caregivers can take to treat nosebleeds.
- Make sure your loved one is well-hydrated especially during colder and dryer months. Around winter time, the weather is colder and the air is dry. People tend to have more nosebleeds at this time. Making sure your loved one is hydrated will keep their lips and nose hydrated and prevent bleeding.
- A sinus infection should be treated with the right medications to make sure it does not cause other problems. See a doctor about proper treatment.
- If your loved one is on aspirin or blood thinners, find out from your loved ones’ doctor what they would recommend to prevent and stop the bleeding.
- Minimize the probability of falls around the home to prevent injuries.
Beyond these, it is always to watch out for other changes that have accompanied the nosebleeds.
This will give you clues as to the actions you should take and when it is time to see a medical professional.
The advantages of companions for the elderly.
As loved ones age, you may notice that they increasingly need someone with stay with them.
Because of reduced mobility and health issues, your elderly loved one may have difficulty moving around and performing normal activities like going to the grocery store.
As more and more people age in place – this means more people are opting to live in their homes rather than a nursing home or assisted living community – the need for a sitter or companion may increase.
And this is especially true when you have to go to work and cannot afford to stay home with your loved one to meet their needs.
Having a sitter or companion in this instance is a great idea.
If you’ve noticed that your loved one has reached a point where they could benefit from a sitter/companion, here is what you can expect.
Companions for the elderly: how companions help
Hiring a companion means you don’t have to worry while you’re at work (or if you live apart from them) that your loved one is being helped.
Here are all the ways a companion can help your loved one.
Transportation Assistance
Does your loved one need to get to a doctor’s appointment? A companion can help them get to the appointment. Do they need to get groceries? A companion can help with that too.
At Green Tree Home Care for instance, our companions will drive your loved one to the places they need to go.
To ensure the safety of your loved one, make sure the company you are hiring companions from is licensed and therefore has insurance that covers driving services.
Light housekeeping
If your loved one needs help with their laundry, companions can help with that. If they need help with keeping their house clean, companions can help as well.
Communication assistance
As the years progress the technology to communicate with friends and family also progresses. It can be frustrating for an older person who is not conversant with these technologies to communicate with family when they need to.
A companion can assist your loved one with communication technologies so that they can stay in touch.
Companionship
This is perhaps the aspect that companions and clients alike love the most – the companionship that develops.
As social beings, we crave relationships and the benefits that come with those relationships.
Companions can accompany your loved one to movies, social events, while they are traveling, to exercise and so much more. These meaningful relationships can help the elderly live longer because it gives them a sense of purpose.
Aging in place is possible. And if you find that your loved one needs more help, they want to remain at home and there are few age-related health issues, you should consider a companion for them.